The Essential Infant CPR & First Aid Course Every New Parent Needs
Gain life-saving confidence without sitting through a dull eight-hour classroom.
Learn Infant CPR, Choking Relief & First Aid Skills That Give You Peace of Mind!
CLICK BELOW TO WATCH FIRST!

4.9/5 star reviews
Thousands of happy customers worldwide
AS SEEN ON
Learn Life-Saving Skills for Your Baby in Just a Few Hours
Does this sound like you?
Panic sets in because you don’t know how to help a choking baby.
Uncertainty about what items belong in a proper infant first aid kit.
Fear of performing CPR incorrectly and causing harm.
Confusion when deciding if a fever requires the ER or simple home care.
Overwhelmed by contradictory safety advice online.
Follow our simple 3-step emergency checklist.
Master life-saving CPR and choking relief in minutes.
Download printable guides for quick reference.
Stock your kit with only our vetted, budget-friendly supplies.
Share your new skills with grandparents and babysitters effortlessly.
What’s Included with Your Enrollment

Infant Anatomy & Safety Basics
Understand how an infant’s body differs and why specialized CPR is critical.

Performing Infant CPR
Grasp the exact hand positions, compression depth and rhythm for effective infant CPR.

Choking Rescue Techniques
Learn immediate actions to clear a blocked airway and stop choking within seconds.

Everyday Infant First Aid
Treat cuts, burns, fevers and allergic reactions with items already in your home.

Emergency Preparedness Plan
Assemble a grab-and-go kit and create an emergency action plan the whole family understands.

Baby-Proofing & Accident Prevention
Prevent the most common household accidents before they happen.
TESTIMONIALS
What our students are saying...

" As a first-time mom I was terrified of choking incidents. After finishing this course I saved my 7-month-old when he coughed up a grape skin. I can’t thank you enough! "
- Emily Johnson


" My wife and I watched the modules in one evening. The instruction is clear, concise, and empowering. We feel so much more confident now. "
- John Doe


" I’m a grandma babysitting twins twice a week. The refresher quizzes kept me sharp and the printable guide stays on our fridge. "
- Roberta Johnson

MODULES
FOLLOW MY STEP BY STEP VIDEO TRAINING
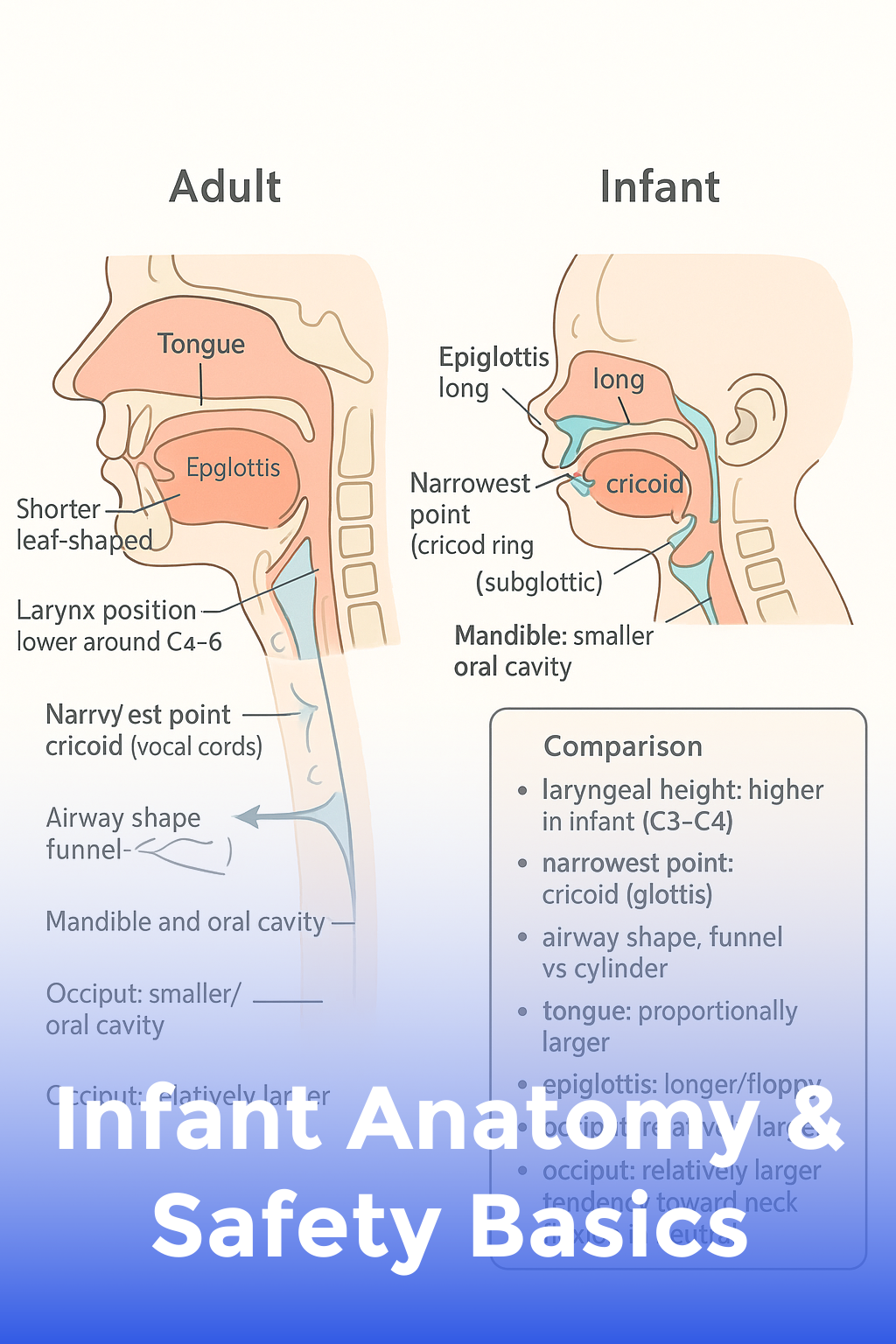
Infant Anatomy & Safety Basics
Understand how an infant’s body differs and why specialized CPR is critical.

Performing Infant CPR
Grasp the exact hand positions, compression depth and rhythm for effective infant CPR.
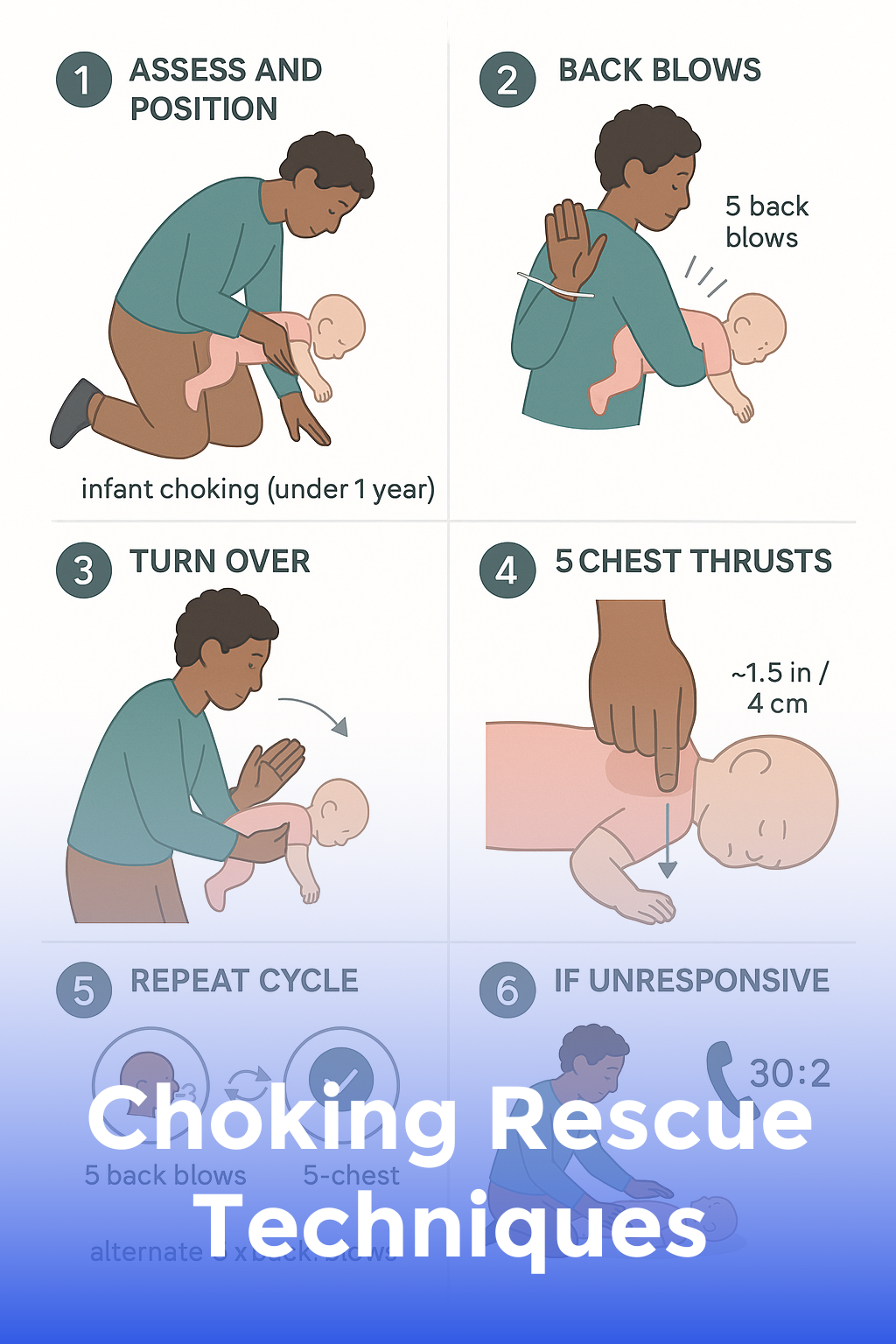
Choking Rescue Techniques
Learn immediate actions to clear a blocked airway and stop choking within seconds.

Everyday Infant First Aid
Treat cuts, burns, fevers and allergic reactions with items already in your home.

Emergency Preparedness Plan
Assemble a grab-and-go kit and create an emergency action plan the whole family understands.

Baby-Proofing & Accident Prevention
Prevent the most common household accidents before they happen.
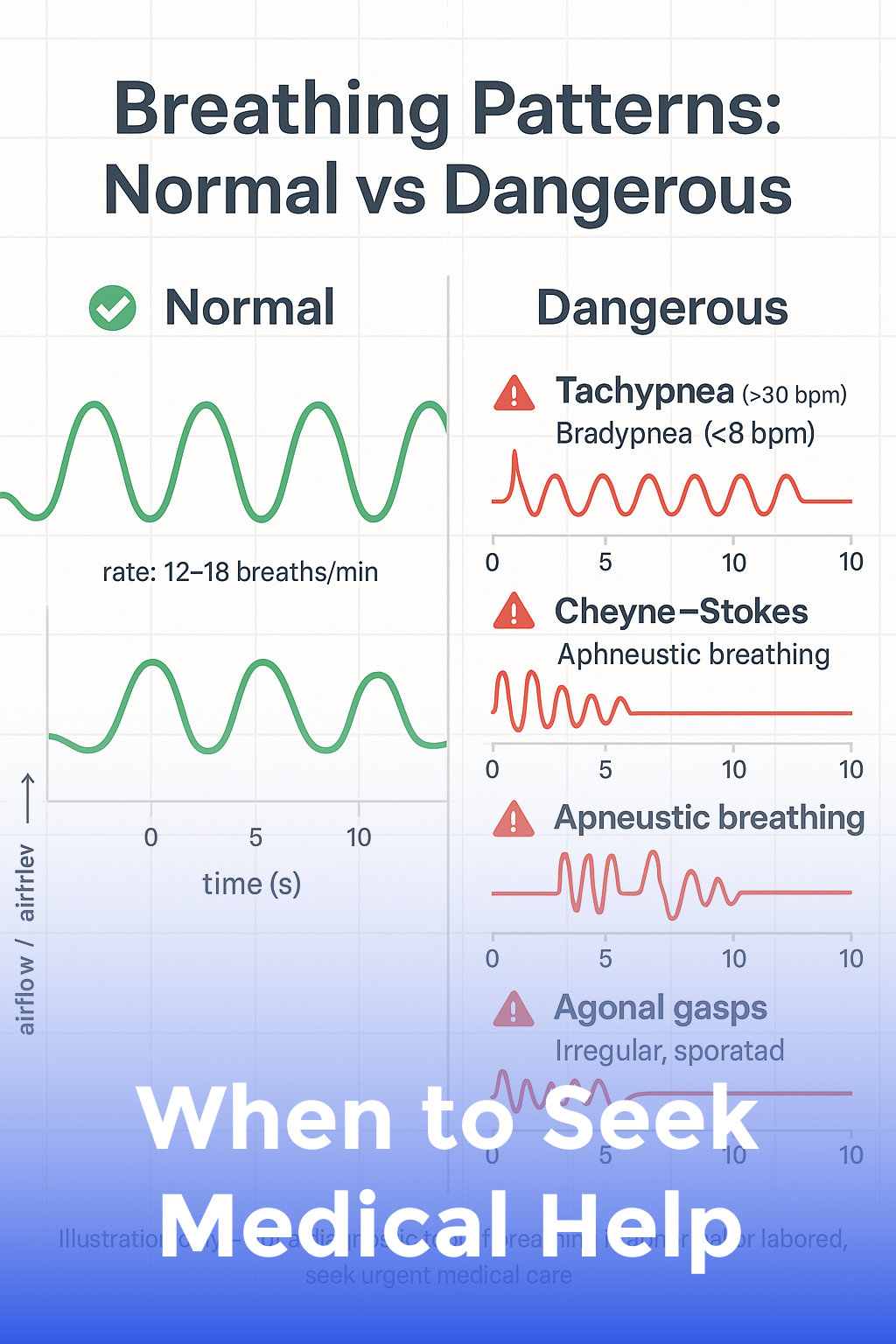
When to Seek Medical Help
Recognize early warning signs of illness and know when to call 911 or the pediatrician.

Staying Calm in Crisis
How to stay calm under pressure using proven stress-management techniques.

4.9/5 star reviews
Feel Confident Handling Any Infant Emergency
Step-by-step video training that teaches you how to respond quickly and calmly when your baby needs help.
Here's what you get:
Instant streaming access to 25 bite-sized HD lessons.
Printable step-by-step CPR & choking wall chart.
Invitation to a private Facebook group of safety-minded parents.
Lifetime updates aligned with the latest American Heart Association guidelines.
Today Just
$997 one time

"Best purchase ever!"
" My wife and I watched the modules in one evening. The instruction is clear, concise, and empowering. We feel so much more confident now. "
ABOUT YOUR INSTRUCTOR
Meet Michael
Taught by a certified pediatric nurse and mother of two who has spent over a decade in children’s emergency care, guiding thousands of families to safety.
After witnessing preventable tragedies in the ER, she realized most parents never receive practical hands-on training and set out to create an accessible, engaging course that empowers families.
Graduates leave knowing exactly what to do during choking, breathing and injury emergencies—many have already saved lives using techniques learned here.
Certified Pediatric Advanced Life Support (PALS) Instructor.
Over 12 years of experience in top children’s hospitals.
Trained more than 5,000 parents and caregivers in CPR.
Featured speaker at national child-safety conferences.
Author of the best-selling guide “Baby Safe at Home.”
Founder of the popular parenting safety blog 'Tiny Hearts, Big Safety'.

WHO IS THIS FOR...
Perfect for expecting parents, new moms and dads, grandparents, babysitters, and anyone caring for infants.
Expecting Moms & Dads
New Parents
Grandparents
Babysitters & Nannies
Daycare Providers
Adoptive & Foster Parents
Pediatric Volunteers
Anyone Caring for Infants
STILL NOT SURE?
Satisfaction guaranteed
We want you to find value in our trainings! We offer full refunds within 30 days. With all of our valuable video training, we are confident you WILL love it!

STILL GOT QUESTIONS?
Frequently Asked Questions
Is this course based on current AHA guidelines?
Absolutely. All techniques follow the latest American Heart Association and Red Cross recommendations and will be updated whenever protocols change.
Do I need any medical background?
No medical experience required! The lessons are beginner-friendly and jargon-free, designed specifically for parents and caregivers.
How long will it take to finish the course?
Most families complete the entire program in under 2 hours, and you can revisit any lesson whenever you need a refresher.
Enroll in the course now!
Copyrights 2024 | Baby Safe Academy™ | Terms & Conditions